A joint team led by Professor Kai Wang from the Zhejiang University International Institutes of Medicine (ZJU-IIM) and Researcher Jian Liu from the centre for Infection Immunity and Cancer (lIC)of Zhejiang University-University of Edinburgh Institute (ZJU-UoE Institute) has published a study in EMBO Molecular Medicine titled “A Monocyte-centered Framework for Predicting Immunochemotherapy Efficacy in Lung Squamous Cell Carcinoma Patients”. The work proposes a clinically applicable, monocyte-centered biomarker framework for predicting treatment response in LUSC.

LUSC accounts for 20%-30% of lung cancers, and targeted therapy options remain limited due to the absence of targetable oncogenic drivers. While neoadjuvant immunochemotherapy has become the standard first-line treatment for locally advanced LUSC, only 24%-50% of patients derive significant benefit from this approach. As a result, there is an urgent need for reliable predictive indicators to guide personalized treatment decisions.
To address this critical gap, the research team utilized paired pre- and post-treatment samples alongside single-cell multi-omics analysis. Through this approach, they identified three key monocyte-related features that correlate with better treatment response: higher monocyte proportion in peripheral blood, higher classical monocyte (CD14⁺CD16⁻) proportion in tumor tissue, and higher APOBEC3A-positive monocyte proportion in both sites. Additionally, single-cell regulatory network analysis (SCENIC) revealed that IRF7 may act as an upstream regulator of APOBEC3A in monocytes, which links to antiviral responses and type I interferon signaling pathways.
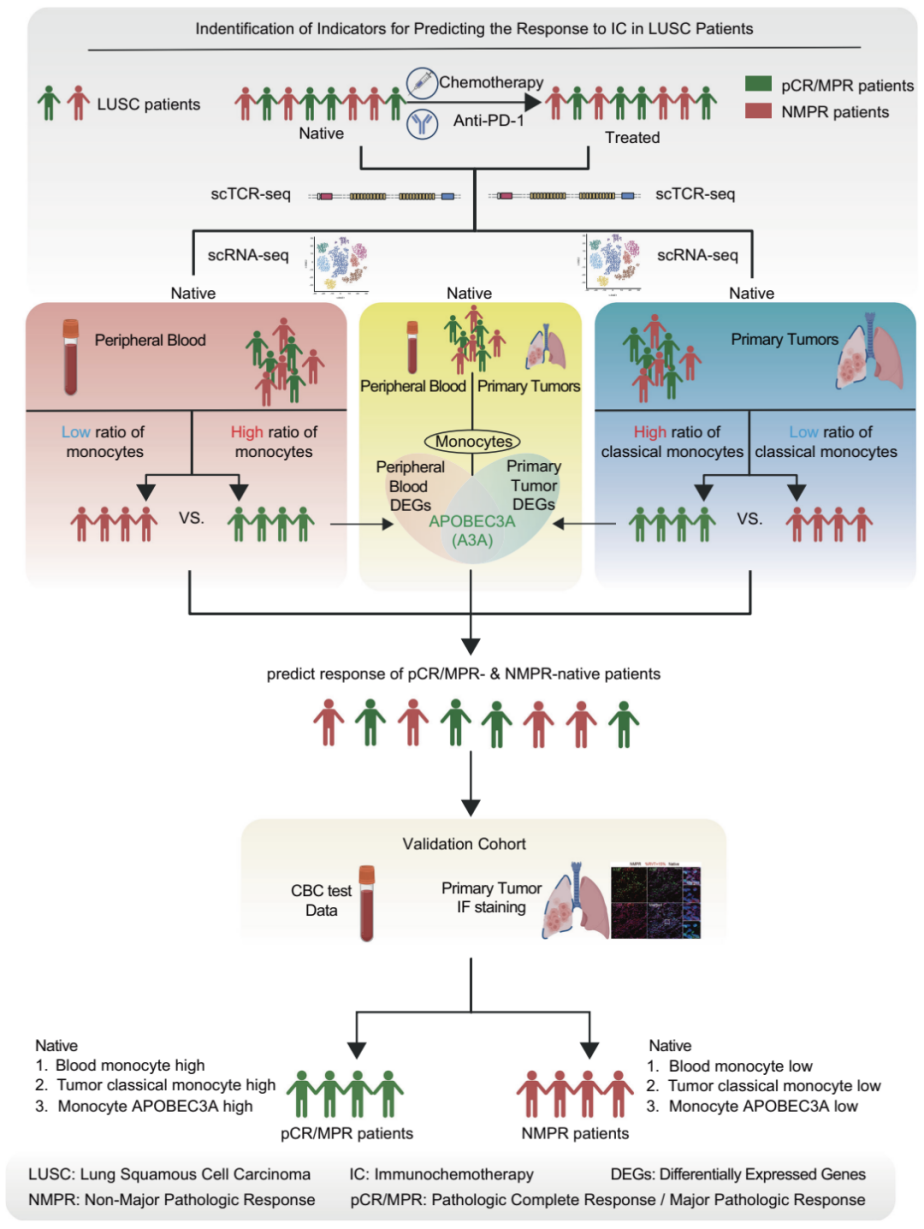
Notably, the peripheral blood monocyte ratio—one of the core indicators—can be directly calculated from routine blood tests, offering a minimally invasive, low-cost option that can be seamlessly integrated into existing clinical workflows. This breakthrough effectively overcomes the limitations of traditional single indicators such as PD-L1 expression and tumor mutational burden (TMB), while also revealing the role of the systemic-tumor monocyte axis in immunochemotherapy efficacy. Collectively, these findings lay a solid foundation for more precise, personalized treatment strategies for LUSC.
Link to the full article:
https://link.springer.com/article/10.1038/s44321-026-00410-y